Introduction:
Varicose veins, a prevalent condition globally, afflict millions, bringing discomfort, pain, and aesthetic unease. Typically seen in the legs, these dilated, contorted veins can severely disrupt daily life. Yet, strides in medical technology offer hope through improved, minimally invasive treatments. Endovenous laser treatment (EVLT), in particular, revolutionises varicose vein care. Unlike traditional surgical methods, EVLT targets affected veins directly with laser energy, sealing them shut. This approach not only reduces recovery time but also minimises scarring and discomfort associated with conventional procedures. Consequently, individuals grappling with varicose veins can now undergo treatment with greater ease and confidence, enhancing their overall well-being. As EVLT continues to gain traction, it underscores a promising shift towards more patient-friendly interventions in managing this widespread vascular issue. If you’re seeking treatment options, consider consulting a varicose veins doctor in Panvel to explore how EVLT could benefit you.
Understanding Varicose Veins and Their Impact:
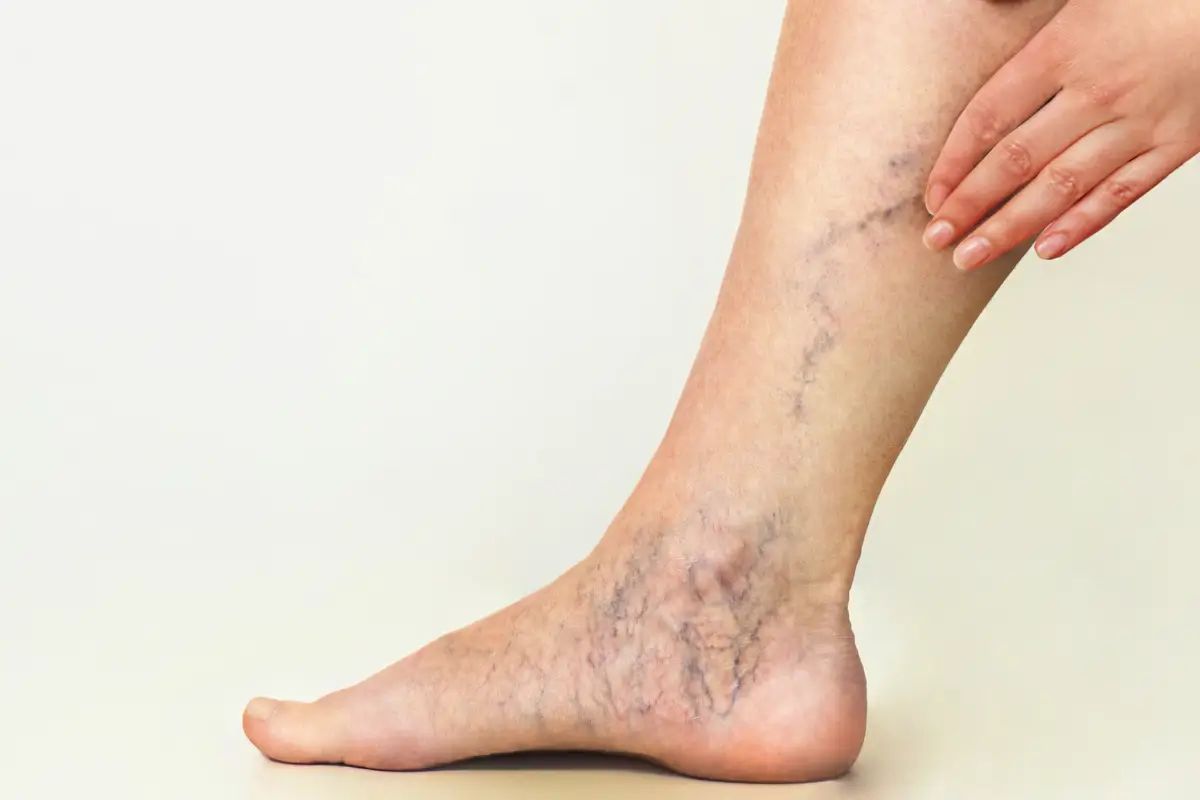
Varicose veins manifest when the valves regulating blood flow in the veins malfunction, leading to blood accumulation and the subsequent bulging and twisting of the veins. This condition is influenced by various factors including genetic predisposition, advancing age, pregnancy, obesity, and prolonged periods of standing or sitting. The hallmark of varicose veins is the visible protrusion of veins, often accompanied by discomfort such as pain, swelling, heaviness, and leg cramps. These symptoms can impact daily activities and diminish quality of life for affected individuals. While primarily a cosmetic concern for some, varicose veins can progress to more serious complications if left untreated, underscoring the importance of early diagnosis and appropriate management to alleviate symptoms and prevent complications.
Traditional Treatment Methods and Their Limitations:
Historically, varicose veins were frequently addressed through surgical techniques such as vein stripping and ligation. Despite their effectiveness, these methods came with notable drawbacks. Patients endured considerable pain, prominent scarring, and prolonged recovery periods. General anaesthesia and hospital stays were often necessary, further increasing the discomfort and inconvenience. These traditional approaches not only imposed physical burdens but also emotional stress on patients. Moreover, they carried risks of complications associated with invasive procedures. Recognizing these challenges, medical advancements have led to the development of minimally invasive treatments like endovenous laser therapy and radiofrequency ablation. These modern techniques offer comparable efficacy with reduced pain, minimal scarring, and shorter recovery times. Patients can now undergo treatment as outpatient procedures, enhancing convenience and reducing overall healthcare costs. Thus, the evolution from conventional surgeries to minimally invasive interventions has significantly improved the management of varicose veins, prioritising patient comfort and well-being.
The Emergence of Endovenous Laser Treatment (EVLT):
In recent years, the advent of endovenous laser treatment (EVLT) has transformed the landscape of varicose vein management. This minimally invasive procedure presents patients with a notably safer, swiffer, and more comfortable option compared to conventional surgery. EVLT operates by harnessing laser energy to effectively seal off the problematic vein, thereby rerouting blood flow towards adjacent, healthier vessels. By obviating the need for extensive incisions and general anaesthesia, EVLT minimises both patient discomfort and recovery time. Furthermore, its precision targeting of affected veins reduces the risk of complications and enhances overall treatment outcomes. As a result, EVLT has become a preferred choice for many individuals seeking relief from the symptoms and aesthetic concerns associated with varicose veins, ushering in a new era of convenience and efficacy in vascular care.
How EVLT Works:
The EVLT (Endovenous Laser Ablation Therapy) procedure involves the insertion of a slender laser fibre into the affected vein through a minor incision. Upon placement, the laser emits controlled energy bursts, effectively heating and causing the collapse of the vein’s walls. This process initiates the body’s natural response to absorb the treated vein gradually. Consequently, blood flow redirects through healthier surrounding veins. EVLT is commonly conducted with local anaesthesia in an outpatient environment, facilitating patients’ same-day discharge and return to their homes. This minimally invasive approach offers a swift recovery period and significantly reduces the risk associated with traditional vein surgeries, making it a preferred choice for managing venous disorders.
Benefits Over Traditional Surgical Methods:
EVLT offers several advantages over traditional surgical techniques, including:
– Minimally invasive: EVLT requires only a tiny incision, reducing trauma to surrounding tissues and minimising scarring.
– Quick recovery: Most patients can resume normal activities within a day or two after the procedure, compared to weeks of downtime with surgery.
– Less pain and discomfort: EVLT causes minimal discomfort during and after the procedure, with most patients experiencing only mild bruising or soreness.
– High success rate: Studies have shown that EVLT is highly effective in treating varicose veins, with low rates of recurrence and complications.
Patient Experience:
Before undergoing Endovenous Laser Ablation (EVLT), patients can anticipate a comprehensive evaluation conducted by a vascular specialist to ascertain the extent of their condition and identify the optimal treatment strategy. Throughout the procedure, patients might experience a slight tingling sensation or warmth as the laser is initiated, though discomfort is generally minimal. Following the procedure, the use of compression stockings may be advised to facilitate healing and alleviate swelling. This post-treatment measure aims to enhance circulation and minimise postoperative complications. Overall, patients can expect a meticulous assessment, a relatively comfortable procedure, and postoperative guidance to promote a smooth recovery process and optimise outcomes.
Recovery Time and Potential Side Effects:
Recovery from Endovenous Laser Treatment (EVLT) is generally swift, allowing patients to return to their routine activities promptly, often within a day or two. A qualified varicose veins doctor in Panvel can provide comprehensive care throughout the process. While mild side effects like bruising, swelling, or tenderness at the treated area may arise, they typically dissipate within a few days. Serious complications such as infection, nerve damage, or blood clots are uncommon but necessitate vigilance. The procedure’s effectiveness in addressing venous issues often outweighs the risks, and adherence to post-treatment care guidelines can mitigate adverse outcomes. Nonetheless, patients should remain aware of potential complications and promptly consult their healthcare provider if any concerning symptoms arise. Overall, EVLT offers a favorable balance of minimal recovery time and low incidence of severe complications, making it a preferred choice for many individuals seeking relief from venous insufficiency.
Effectiveness and Safety:
Numerous studies have confirmed the effectiveness and safety of Endovenous Laser Ablation Therapy (EVLT) in the management of varicose veins. Extensive research consistently reveals impressive success rates in vein closure and alleviation of symptoms, coupled with minimal recurrence and complications. Compared to conventional surgical interventions, EVLT provides comparable therapeutic outcomes while substantially reducing associated risks and discomfort. This minimally invasive approach harnesses laser energy to target and seal off problematic veins, offering patients a less invasive and more comfortable alternative to traditional surgical procedures. The evidence underscores EVLT as a reliable and patient-friendly option for treating varicose veins, promising improved clinical outcomes and enhanced quality of life for individuals seeking relief from this common vascular condition.
Cost Considerations:
While the upfront expense of Endovenous Laser Treatment (EVLT) may surpass that of traditional surgery, its long-term cost-effectiveness is noteworthy. Numerous insurance plans recognize EVLT as medically necessary for symptomatic varicose veins, thereby diminishing patients’ out-of-pocket costs. Additionally, finding a skilled varicose veins doctor in Panvel to perform EVLT can ensure optimal outcomes. Furthermore, EVLT’s shorter recovery duration and reduced likelihood of complications translate to savings on post-operative care and subsequent appointments. The initial investment in EVLT pales in comparison to the cumulative expenses associated with conventional surgery, making it a financially prudent choice over time. This not only eases the financial burden on patients but also underscores the economic viability of EVLT as a preferable treatment option for varicose veins.
Conclusion:
Endovenous laser treatment (EVLT) stands out as a revolutionary approach to treating varicose veins, revolutionising how patients manage this condition. Unlike traditional surgery, EVLT offers a notably safer, more comfortable, and less invasive option. Its impressive success rates, coupled with rapid recovery times and minimal side effects, signify a remarkable leap forward in vascular medicine. By comprehending the advantages of EVLT and its potential impact on varicose vein treatment, patients gain the knowledge necessary to make informed healthcare decisions. Ultimately, embracing EVLT translates to improved outcomes and an enhanced quality of life for individuals grappling with varicose veins. If you’re seeking expert care for varicose veins in Panvel, consider consulting with a varicose veins doctor in Panvel to explore EVLT as a viable treatment option.